 Your new post is loading...
 Your new post is loading...
Wearables that have weaved their way into everyday life include smart watches and wireless earphones, while in the healthcare setting, common devices include wearable injectors, electrocardiogram (ECG) monitoring patches, listening aids, and more. A major pain point facing the use of these wearables is the issue of keeping these devices properly and conveniently powered. As the number of wearables one uses increases, the need to charge multiple batteries rises in tandem, consuming huge amounts of electricity. A research team, led by Associate Professor Jerald Yoo from the Department of Electrical and Computer Engineering and the N.1 Institute for Health at the National University of Singapore (NUS), has developed a technology that enables a single device, such as a mobile phone placed in the pocket, to wirelessly power other wearable devices on a user's body, using the human body as a medium for power transmission. The team's novel system has an added advantage—it can harvest unused energy from electronics in a typical home or office environment to power the wearables. The NUS team designed a receiver and transmitter system that uses the human body as a medium for power transmission and energy harvesting. Each receiver and transmitter contains a chip that is used as a springboard to extend coverage over the entire body. A user just needs to place the transmitter on a single power source, such as the smart watch on a user's wrist, while multiple receivers can be placed anywhere on the person's body. The system then harnesses energy from the source to power multiple wearables on the user's body via a process termed as body-coupled power transmission. In this way, the user will only need to charge one device, and the rest of the gadgets that are worn can simultaneously be powered up from that single source. The team's experiments showed that their system allows a single power source that is fully charged to power up to 10 wearable devices on the body, for a duration of over 10 hours. As a complementary source of power, the NUS team also looked into harvesting energy from the environment. Their research found that typical office and home environments have parasitic electromagnetic (EM) waves that people are exposed to all the time, for instance, from a running laptop. The team's novel receiver scavenges the EM waves from the ambient environment, and through a process referred to as body-coupled powering, the human body is able to harvest this energy to power the wearable devices, regardless of their locations around the body. This paves the way for smaller, battery-free wearables read the paper in Nature at http://dx.doi.org/10.1038/s41928-021-00592-y read the original unedited article https://techxplore.com/news/2021-06-approach-wirelessly-power-wearable-devices.html
A team of researchers has developed the first human "mini-hearts" in the lab to have clearly beating chambers. The miniature organs, or organoids, are no bigger than sesame seeds and were generated by self-assembly using pluripotent stem cells, according to Science Magazine. The organoids mimic the functioning heart of a 25-day-old human embryo, and they may help humans solve the heart's many mysteries. Our capability to model the complexity of the human heart in vitro is still limited, consequently limiting our knowledge of how heart diseases develop. Congenital heart defects, for example, are the most common birth condition in humans, affecting around 1 percent of all live births. This alone demonstrates the need to create more precise organ-like platforms, which is where the researchers come in, with their newly devised method which was described in a study published in the journal Cell. The researchers engineered human pluripotent stem cells, which can divide into any kind of tissue, into multiple forms of cardiac cells to create heart organoids whose cells self-organize like those in an embryo. The aim was to create three tissue layers that make up a heart chamber's walls, which are one of the first parts of the heart to form. The organoids, which are around 2 mm in diameter and have survived more than 3 months in the lab so far, become structurally equal to the heart of a 25-year-old embryo in a week. They only have one chamber and the main types of cells at this point of development. Moreover, the heart's clearly defined chamber beats 60 to 100 times a minute, much like the heart of an embryo at the same age. read the entire story at https://interestingengineering.com/lab-grown-mini-heart-beats-like-a-25-day-old-human-embryos-heart
The use of technology in health care has proven to increases care providers, the capabilities and to patients, access to improved quality of healthcare. During the GDD summit organized by BAO Systems, it occurred that some of the most beneficial countries include Nigeria. Speaking at the summit, InStrat Global Health Solution (InStratGHS) CEO, Okey Okuzu, discussed the design, deployment, and impact of Artificial Intelligence (AI) tool – EWORS for TB case finding in Nigeria. EWORS is built on the MediXcel Digital Health Platform by Plus91 “Our goal is to overcome barriers to healthcare delivery in low resource settings presented by infrastructural challenges,” he noted. “We achieve this by leveraging mobile health technologies that allow for smooth flow of information across the health system for more effective patient health management or policy decisions regardless of physical location.” The MediXcel-EWORS system is designed to drive actionable AI for public health intervention by sieving through a large volume of data to enable specific geospatial identification of disease cases and also predict the possibility of an outbreak based on historical data and set algorithm threshold. This helps local surveillance personnel to make data-informed decisions to curb the spread of diseases. Field data, captured on android devices wirelessly transferred to a cloud server for storage and analysis. “The EWORS engine conducts advanced analytics to detect unexpected elevations in indicator data and populates this information on real-time GIS heat maps, reports, and alert notifications,” he added. The alert notifications are generated in form of emails/SMS and sent to designated individuals when data from local areas exceed set thresholds, indicating undetected community spread. Designated teams review alarms and mobilize to conduct mass screening outreach at Alarm locations. Under a USAID-funded program led by the KNCV TB Foundation, and in partnership with Plus91 PVT, InStrat GHS deployed its EWORS predictive engine to 14 Nigerian states as a solution to find undetected TB cases in the country. The Analyses of the data from program inception to date demonstrate that prioritization of case finding outreach efforts, based on hotspot analytics and alarms, increases the yield of those efforts. This strategy is crucial to finding missing TB cases and improving case-finding, especially in low resource settings, read more at https://www.cio.co.ke/role-of-ai-in-healthcare-tb-prevalence-in-nigeria/ read about Instrats at https://instratghs.com/ read about Plus91 and MediXcel at https://plus91.in/about-us/ read about KCNV at https://kncvnigeria.org/
Two scientific leaps, in machine learning algorithms and powerful biological imaging and sequencing tools , are increasingly being combined to spur progress in understanding diseases and advance AI itself. Cutting-edge, machine-learning techniques are increasingly being adapted and applied to biological data, including for COVID-19. Recently, researchers reported using a new technique to figure out how genes are expressed in individual cells and how those cells interact in people who had died with Alzheimer's disease. Machine-learning algorithms can also be used to compare the expression of genes in cells infected with SARS-CoV-2 to cells treated with thousands of different drugs in order to try to computationally predict drugs that might inhibit the virus. While, Algorithmic results alone don't prove the drugs are potent enough to be clinically effective. But they can help identify future targets for antivirals or they could reveal a protein researchers didn't know was important for SARS-CoV-2, providing new insight on the biology of the virus read the original article which speaks about a lot more at https://www.axios.com/ai-machine-learning-biology-drug-development-b51d18f1-7487-400e-8e33-e6b72bd5cfad.html
Cancer is next problem to tackle with mRNA tech, says BioNTech founder
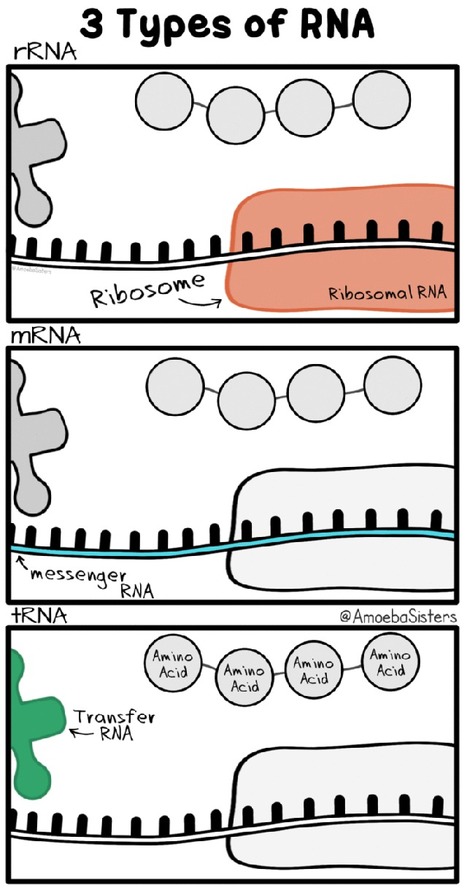
The co-founder of German company BioNTech, which successfully delivered the first widely distributed coronavirus vaccine, said that the mRNA technology it used will soon be put to work tackling cancer. Özlem Türeci, who started BioNTech alongside her husband, said that she had been working to use the body's immune system to combat cancer tumors before the coronavirus pandemic stopped the world. “We have several different cancer vaccines based on mRNA,” The coronavirus vaccine made by BioNTech(and also Pfizer) uses messenger RNA, or mRNA, to deliver instructions to the body to make proteins that will alert it to attack a certain virus. The same technology can in theory be used for cancer tumors. What is mRNA ? Messenger RNA (mRNA) is a single-stranded RNA molecule that is complementary to one of the DNA strands of a gene. The mRNA is an RNA version of the gene that leaves the cell nucleus and moves to the cytoplasm where proteins are made. During protein synthesis, an organelle called a ribosome moves along the mRNA, reads its base sequence, and uses the genetic code to translate each three-base triplet, or codon, into its corresponding amino acid.
The mRNA Approach to Vaccines
mRNA vaccines are a new type of vaccine to protect against infectious diseases. To trigger an immune response, many vaccines put a weakened or inactivated germ into our bodies. Not mRNA vaccines. Instead, they teach our cells how to make a protein—or even just a piece of a protein—that triggers an immune response inside our bodies. That immune response, which produces antibodies, is what protects us from getting infected if the real virus enters our bodies. mRNA vaccines have been studied before for flu, Zika, rabies, and cytomegalovirus (CMV). As soon as the necessary information about the virus that causes COVID-19 was available, scientists began designing the mRNA instructions for cells to build the unique spike protein into an mRNA vaccine. Future mRNA vaccine technology may allow for one vaccine to provide protection for multiple diseases, thus decreasing the number of shots needed for protection against common vaccine-preventable diseases.
Imagine you’re a scientist who needs to discover a new antibiotic to fight off a scary disease. How would you go about finding it? Typically, you’d have to test lots and lots of different molecules in the lab until you find one that has the necessary bacteria-killing properties. You might find some contenders that are good at killing the bacteria only to realize that you can’t use them because they also prove toxic to humans. It’s a very long, very expensive, and probably very aggravating process. But what if, instead, you could just type into your computer the properties you’re looking for and have your computer design the perfect molecule for you? That’s the general approach IBM researchers are taking, using an AI system that can automatically generate the design of molecules for new antibiotics. In a new paper, published in Nature Biomedical Engineering, the researchers detail how they’ve already used it to quickly design two new antimicrobial peptides — small molecules that can kill bacteria — that are effective against a bunch of different pathogens in mice. Normally, this molecule discovery process would take scientists years. The AI system did it in a matter of days. That’s great news, because we urgently need faster ways to create new antibiotics. How IBM’s AI system works IBM’s new AI system relies on something called a generative model. To understand it at its simplest level, we can break it down into three basic steps. First, the researchers start with a massive database of known peptide molecules. Then the AI pulls information from the database and analyzes the patterns to figure out the relationship between molecules and their properties. It might find that when a molecule has a certain structure or composition, it tends to perform a certain function. This allows it to “learn” the basic rules of molecule design. Finally, researchers can tell the AI exactly what properties they want a new molecule to have. They can also input constraints (for example: low toxicity, please!). Using this info on desirable and undesirable traits, the AI then designs new molecules that satisfy the parameters. The researchers can pick the best one from among them and start testing on mice in a lab. The IBM researchers claim that their approach outperformed other leading methods for designing new antimicrobial peptides by 10 percent. They found that they were able to design two new antimicrobial peptides that are highly potent against diverse pathogens, including multidrug-resistant K. pneumoniae, a bacterium known for causing infections in hospital patients. Happily, the peptides had low toxicity when tested in mice, an important signal about their safety (though not everything that’s true for mice ends up being generalizable to humans). read the original unedited article at https://www.vox.com/future-perfect/22360573/ai-ibm-design-new-antibiotics-covid-19-treatments read the paper by the IBM researchers - Accelerated antimicrobial discovery via deep generative models and molecular dynamics simulations
|
Purdue University engineers have developed a method to transform existing cloth items into battery-free wearables resistant to laundry. These smart clothes are powered wirelessly through a flexible, silk-based coil sewn on the textile. In the near future, all your clothes will become smart. These smart clothes will outperform conventional passive garments, thanks to their miniaturized electronic circuits and sensors, which will allow you to seamlessly communicate with your phone, computer, car and other machines. This smart clothing will not only make you more productive but also check on your health status and even call for help if you suffer an accident. The reason why this smart clothing is not all over your closet yet is that the fabrication of this smart clothing is quite challenging, as clothes need to be periodically washed and electronics despise water. Purdue engineers have developed a new spray/sewing method to transform any conventional cloth items into battery-free wearables that can be cleaned in the washing machine. "By spray-coating smart clothes with highly hydrophobic molecules, we are able to render them repellent to water, oil and mud," said Ramses Martinez, an assistant professor in Purdue's School of Industrial Engineering and in the Weldon School of Biomedical Engineering in Purdue's College of Engineering. "These smart clothes are almost impossible to stain and can be used underwater and washed in conventional washing machines without damaging the electronic components sewn on their surface." read the study at http://dx.doi.org/10.1016/j.nanoen.2021.106155 read the original and unedited version of the article at https://phys.org/news/2021-06-wearables-future-washable-smart-powered.html
Atypical eye gaze is an early-emerging symptom of autism spectrum disorder (ASD) and holds promise for autism screening. Current eye-tracking methods are expensive and require special equipment and calibration. There is a need for scalable, feasible methods for measuring eye gaze. This case-control study examines whether a mobile app that displays strategically designed brief movies can elicit and quantify differences in eye-gaze patterns of toddlers with autism spectrum disorder (ASD) vs those with typical development. In effect, using computational methods based on computer vision analysis, can a smartphone or tablet be used in real-world settings to reliably detect early symptoms of autism spectrum disorder? Findings In this study, a mobile device application deployed on a smartphone or tablet and used during a pediatric visit detected distinctive eye-gaze patterns in toddlers with autism spectrum disorder compared with typically developing toddlers, which were characterized by reduced attention to social stimuli and deficits in coordinating gaze with speech sounds. What this means These methods may have potential for developing scalable autism screening tools, exportable to natural settings, and enabling data sets amenable to machine learning. Conclusions and Relevance The app reliably measured both known and new gaze biomarkers that distinguished toddlers with ASD vs typical development. These novel results may have potential for developing scalable autism screening tools, exportable to natural settings, and enabling data sets amenable to machine learning. read the study at https://jamanetwork.com/journals/jamapediatrics/fullarticle/2779395
mRNA is a type of genetic material that tells your body how to make proteins. The two mRNA vaccines for SARS-CoV-2, the coronavirus that causes COVID-19, deliver fragments of this mRNA into your cells. The world’s first mRNA vaccines — the COVID-19 vaccines from Pfizer/BioNTech and Moderna — have made it in record time from the laboratory, through successful clinical trials, regulatory approval and into people’s arms. The high efficiency of protection against severe disease, the safety seen in clinical trials and the speed with which the vaccines were designed are set to transform how we develop vaccines in the future. We have two mRNA COVID-19 vaccines so far. But what else can this technology do? Once researchers have set up the mRNA manufacturing technology, they can potentially produce mRNA against any target. Manufacturing mRNA vaccines also does not need living cells, making them easier to produce than some other vaccines. So mRNA vaccines could potentially be used to prevent a range of diseases, not just COVID-19. Flu vaccine Moderna is already turning its attention to an mRNA vaccine against seasonal influenza. This would target the four seasonal strains of the virus the WHO predicts will be circulating. But the holy grail is a universal flu vaccine. This would protect against all strains of the virus (not just what the WHO predicts) and so wouldn’t need to be updated each year. The same researchers who pioneered mRNA vaccines are also working on a universal flu vaccine. Malaria vaccine There is no vaccine for Malaria. However, US researchers working with pharmaceutical company GSK have filed a patent for an mRNA vaccine against malaria. The mRNA in the vaccine codes for a parasite protein called PMIF. By teaching our bodies to target this protein, the aim is to train the immune system to eradicate the parasite. This malaria mRNA vaccine is an example of a self-amplifying mRNA vaccine. This means very small amounts of mRNA need to be made, packaged and delivered, as the mRNA will make more copies of itself once inside our cells. This is the next generation of mRNA vaccines after the “standard” mRNA vaccines seen so far against COVID-19. Cancer vaccines We already have vaccines that prevent infection with viruses that cause cancer. For example, hepatitis B vaccine prevents some types of liver cancer and the human papillomavirus (HPV) vaccine prevents cervical cancer. But the flexibility of mRNA vaccines lets us think more broadly about tackling cancers not caused by viruses. Some types of tumours have antigens or proteins not found in normal cells. If we could train our immune systems to identify these tumour-associated antigens then our immune cells could kill the cancer. Cancer vaccines can be targeted to specific combinations of these antigens. BioNTech is developing one such mRNA vaccine that shows promise for people with advanced melanoma. CureVac has developed one for a specific type of lung cancer, with results from early clinical trials. Then there’s the promise of personalised anti-cancer mRNA vaccines. If we could design an individualised vaccine specific to each patient’s tumour then we could train their immune system to fight their own individual cancer. Several research groups and companies are working on this. read the unedited original article at https://theconversation.com/3-mrna-vaccines-researchers-are-working-on-that-arent-covid-157858
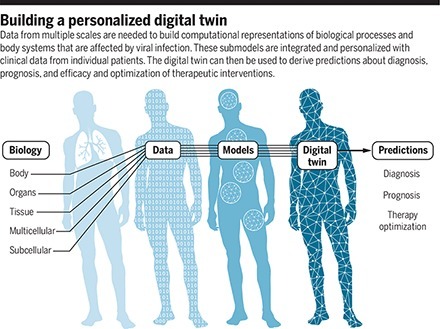
No current tool can predict the course of disease and help a doctor decide on the most appropriate treatment for an individual COVID-19 patient. Digital twins are software replicas of the dynamic function and failure of engineered products and processes. The medical analog, patient-specific digital twins, could integrate known human physiology and immunology with real-time patient-specific clinical data to produce predictive computer simulations of viral infection and immune response. Such medical digital twins could be a powerful addition to our arsenal of tools to fight future pandemics, combining mechanistic knowledge, observational data, medical histories, and the power of artificial intelligence (AI). Although medical digital twins are much more difficult to develop than those for engineered devices, they have begun to find applications in improving human health. Examples include the “artificial pancreas” for type 1 diabetes patients Building a personalized digital twin Data from multiple scales are needed to build computational representations of biological processes and body systems that are affected by viral infection. These submodels are integrated and personalized with clinical data from individual patients. The digital twin can then be used to derive predictions about diagnosis, prognosis, and efficacy and optimization of therapeutic interventions. Digital twins describing infection and treatment require the development, validation, and integration of numerous component submodels in the context of a rapidly developing scientific understanding of biological behaviors and continual generation of new experimental and clinical data. Although individual laboratories may construct submodels, the development of comprehensive digital twins will require laboratories and research groups around the world to integrate and validate submodels independently, with only limited central coordination. Enabling such parallel development requires a flexible simulation architecture that uses a multiscale map of all the relevant components of a patient's response to viral infection, as well as responses to available treatments. read the paper at https://science.sciencemag.org/content/371/6534/1105.full
Many viruses infect their hosts through mucosal surfaces such as the lining of the respiratory tract. MIT researchers have now developed a vaccination strategy that can create an army of T cells that are ready and waiting at those surfaces, offering a quicker response to viral invaders. The researchers showed that they could induce a strong memory T cell response in the lungs of mice by giving them a vaccine modified to bind to a protein naturally present in mucus. This can help ferry the vaccine across mucosal barriers, such as the lining of the lungs “In this paper, we specifically focused on T cell responses that would be useful against viruses or cancer, and our idea was to use this protein, albumin, as sort of a Trojan horse to get the vaccine across the mucosal barrier,” says Darrell Irvine, the senior author of the study, who is the Underwood-Prescott Professor with appointments in the departments of Biological Engineering and Materials Science and Engineering; an associate director of MIT’s Koch Institute for Integrative Cancer Research; and a member of the Ragon Institute of MGH, MIT, and Harvard. In addition to protecting against pathogens that infect the lungs, these types of inhaled vaccines could also be used to treat cancer metastasizing to the lungs or even prevent cancer from developing in the first place, the researchers say. read the release from the MIT news Office at https://news.mit.edu/2021/vaccination-inhalation-0319
Vaccination Passports - What are they?
As mass vaccination programs are being rolled out globally, vaccine passports have become a major topic of discussion. COVID test results and proof of vaccine will be required in many countries for quarantine-free travel, just as it has been for polio and yellow fever vaccinations in the past. Countries will need to look at convenient and secure ways for verifying COVID-19 test results and vaccination information at airports and borders. The International Air Transport Association (IATA) has also called for a “global standard to securely record digital proof of vaccination”. They have been promoting the IATA Travel Pass Initiative (https://www.iata.org/en/programs/passenger/travel-pass/) In February, Qantas completed a trial run of an app for this purpose on an international repatriation flight from Frankfurt to Darwin. The idea behind the app is that health or border officials and airline staff may be able to easily verify COVID-19 test results and vaccination history of an individual. The app links customers with certified testing labs to allow their results to be automatically uploaded onto it. Similar digital solutions are being developed in several other countries around the world to enable travel again. For instance, travellers from Singapore will receive a notarized certificate following a negative COVID-19 test that they can present at airports around the world. Another example is France taking part in a month-long trial of a vaccine passport that leverages a smart phone app. Its important that such digital health technologies, whether apps or chip cards, or health tracker add ons, be easy to use. It important that the process be as seamless as possible for flyers share the relevant information as well as get the information validated by the ground and air staff so they people can travel internationally, again, safely! image source: https://foto.wuestenigel.com/person-hands-holding-a-covid-19-passport/ image license: https://creativecommons.org/licenses/by/2.0/
|



 Your new post is loading...
Your new post is loading...
















A part of me smiled and a part of me felt a little scared reading this. Are we looking at the future of us being turned into batteries as shown in the Matrix?
Jokes apart, this is path breaking and can lead to a very sustainable mechanism for the future of wearables, monitoring and diagnostics.