 Your new post is loading...
 Your new post is loading...
Individuals do not have a poor posture on purpose. It becomes a habit that just goes on until discomfort or pain present. Body awareness is known as proprioception. Proprioception is known as muscle sense or joint position sense. This is the subconscious nature of the body's understanding of its position in space and the ability to position ourselves comfortably. Achieving proper and healthy posture means there needs to be a constant mindset of staying aware of how the body is positioned. Then regular adjustments of body position are required to maintain healthy body awareness and from getting into bad habits. To illustrate this consider walking forward in complete darkness. The body knows its relative position even without seeing and understands its existence in space. This is a function of the brain. It is part of the subconscious and so have little to no control over it. Because of this individuals begin to lapse into poor poster habits. An example tilting the head when looking forward or all the way down when checking the phone. Over time, these bad habits contribute to spinal misalignment. This is where chiropractic can help individuals realize their proprioception tendencies and actively relearn and strengthen positive body awareness and break away from negative postural habits. Body Awareness Habits Laying the groundwork for correction of body awareness involves understanding the body's unconscious habits and the damage that is occurring. Chiropractic is highly effective for outlining what is happening with the help of radiological imaging and spinal curvature benchmarks. Once an individual begins to understand how their posture and spine health are being affected, they can make adjustments to combat this. This requires constant vigilance by the individual to actively realize and correct proprioception. Optimal Body Exercises For individuals that have engaged in dysfunctional habits for years, a chiropractor may recommend optimal loading exercises. This process involves teaching how to better balance the body for optimal posture development. For example, a chiropractor will have a patient strengthen a weak leg that is shifting the body's weight to the other dominant leg that results in unbalanced weight distribution causing hip and back pain. Another example of optimal loading may include executing a series of motions/movements with the non-dominant side. The goal of optimal loading is to train the brain to balance the body in a healthier fashion, instead of reverting to a bad habit. Ergonomics Ergonomics can also help correct dysfunctional proprioception. They can help to address specific defaults of the subconscious. For example, the positioning of a computer screen at the correct height and angle can improve the habit of turning or tilting the head. Another example is utilizing custom foot orthotics to balance the feet and prevent pronation. A chiropractor can determine exactly where the ergonomic intervention will have a significant effect in correcting dysfunctional proprioception. Chiropractic Relief Chiropractic postural adjustments, optimal loading exercises, and ergonomics are all recommended tools in rehabilitating and preventing bad posture habits. Injury Medical Chiropractic and Functional Medicine Clinic will explore every possible approach to help patients understand and overcome the body’s bad habits, and help them achieve optimal spine health. Muscles get weaker with too much sitting When sitting the gluteal muscles, abdominal muscles, and legs become dormant. Sitting for extended periods day after day causes these muscles to begin to degenerate. Metabolism is linked with body composition. Having more muscle increases metabolism and helps the body burn more calories. Any muscle loss, especially from the lower body which is the largest muscle group, can lead to progressive fat gain if the diet is not adjusted. With time gradual muscle loss from the lower body can hurt functional strength, and older age increases the risk of falls and affects the quality of life. Dr. Alex Jimenez’s Blog Post Disclaimer The scope of our information is limited to chiropractic, musculoskeletal, physical medicines, wellness, and sensitive health issues and/or functional medicine articles, topics, and discussions. We use functional health & wellness protocols to treat and support care for injuries or disorders of the musculoskeletal system. Our posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate and support directly or indirectly our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. We understand that we cover matters that require an additional explanation as to how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. The provider(s) Licensed in Texas& New Mexico* References Corliss J. Too much sitting linked to heart disease, diabetes, premature death. Harvard Health Blog. http://www.health.harvard.edu/blog/much-sitting-linked-heart-disease-diabetes-premature-death-201501227618. Published January 22, 2015. Accessed January 7, 2017. Ergonomics for Prolonged Sitting. UCLA Spine Center Web site. http://spinecenter.ucla.edu/ergonomics-prolonged-sitting. Accessed January 7, 2017. Florido R, Michos E. Sitting Disease: Moving Your Way to a Healthier Heart. U.S. News & World Report. http://health.usnews.com/health-news/patient-advice/articles/2015/09/14/sitting-disease-moving-your-way-to-a-healthier-heart. Published September 14, 2015. Accessed January 7, 2017.
Low back pain is a common health issue for many people. Nearly everybody will experience lower back pain at any moment in their own lives. This pain can differ from mild to severe and it might be short-term or long-term. When it happens, low back pain can make many everyday tasks difficult to participate and engage in. That all too familiar annoyance, however, can tremendously limit time spent relaxing, working, and even that of relationships. Moreover, low back pain might also lead to irritability as well as a whole onslaught of additional medical health issues if not treated appropriately. The prevalence of low back pain has become a common problem, amounting to one of the most common reasons for doctor office visits each year. Before considering what type of treatment approach to follow for your back pain, it’s important to understand the anatomy of the spine and how low back pain occurs.
Chiropractic care is a well-known alternative treatment option commonly used for a variety of injuries and/or conditions, including low back pain and sciatica. Of course, not all pain is physical nor does it always have a physical cause. Stress, anxiety and depression affects millions of people each year. While many patients require prescription drug therapy to treat their mental health issues, others may be able to control and treat they symptoms with a holistic approach. Chiropractic care is an effective stress management treatment which can help reduce symptoms associated with stress, such as low back pain and sciatica. Most chiropractors will utilize other treatment methods and techniques, such as physical therapy, exercise, and nutrition advice, to further increase the stress management effects of chiropractic care. These lifestyle changes affect every area of your well-being. Furthermore, the purpose of the article below is to demonstrate the effects of mindfulness-based stress reduction compared to cognitive-behavioral therapy and usual care on stress with associated symptoms of chronic low back pain and sciatica.
Low back pain due to lumbar disc herniation (LDH) is very common in clinic. This randomized controlled trial was designed to investigate the effects of integrative TCM conservative therapy for low back pain due to LDH. A total of 408 patients with low back pain due to LDH were randomly assigned to an experimental group with integrative TCM therapy and a control group with normal conservative treatment by the ratio of 3 : 1. The primary outcome was the pain by the visual analogue scale (VAS). The secondary outcome was the low back functional activities by Chinese Short Form Oswestry Disability Index (C-SFODI). Immediately after treatment, patients in the experimental group experienced significant improvements in VAS and C-SFODI compared with the control group (between-group difference in mean change from baseline, −16.62 points, P < 0.001 in VAS; −15.55 points, P < 0.001 in C-SFODI). The difference remained at one-month followup, but it is only significant in C-SFODI at six-month followup (−7.68 points, P < 0.001). No serious adverse events were observed. These findings suggest that integrative TCM therapy may be a beneficial complementary and alternative therapy for patients with low back pain due to LDH.
Pain that travels from the back down the leg and into the foot is known as sciatica, which is an overall expression for pain that is excruciating. The term does not clarify why, or what tissue is injured. In reality accidents can cause gastrointestinal pain, together with piriformis syndrome, lumbar spinal disc herniations, and sprains being the three most frequent types of injuries and conditions affecting health and wellness. Piriformis syndrome is commonly misdiagnosed as a spinal disc herniation, because the pattern of radiating pain, in the back to the lower elevation, is similar in both cases. With both injuries, individuals experience pain with the same type of motions, particularly rising from a seated position, standing for prolonged period of time, or sleeping. At the same time, the pain related to both injuries feels better once you curl up in the fetal position on your side. A spinal disc herniation occurs when the jelly-like substance from inside the lumbar disc compresses the spinal cord or nerve. Either the disc material compresses the nerves when squeezed out of this disc, or else the compression of the nervous tissue is caused by inflammation. A spinal disc herniation is generally considered a severe injury, causing a massive amount of restriction and back pain. Some folks lose sensation in their legs. They can experience numbness and tingling through the day. Several have tingling, burning, dull, or pain in leg, glutes, and their own back. These are all symptoms associated with sciatica. Compression of particular nerves causes muscle fatigue and loss of feeling.
In a first-of-its-kind study, researchers used a real world” strategy that was “ compared to running the study in a managed setting.
More than 50 percent of the research participants reported, “clinically purposeful development” in their low back pain after their massage therapy plan, composed co-first authors William G. Elder, PhD, Family and Community Medicine at the University of Kentucky, and Niki Munk, PhD, LMT, School of Health and Rehabilitation Sciences at Indiana University-Purdue University Indianapolis.
“Clinical massage therapy appears to be effective for low back pain, and patients should discuss with their provider and consider clinical massage therapy before attempting highly debatable opioid drugs,” says Dr. Elder, who was the lead researcher of the study.
Most people don’t go to a chiropractor for a better sex life, but that extra benefits is a pretty happy accident. “People come in with back pain, but after adjustments, they come back and tell me their sex life is so much better,” says Jason Helfrich, co-founder and CEO of 100% Chiropractic. “It’s no surprise to us—it’s amazing what the body will do when you take away the pressure on the nervous system.”
And what are those amazing feats, exactly? Let’s start with what a chiropractor really does. Every function in your body is controlled from the nervous system, but when vertebra are off position—known as a subluxation—the nerves traveling between your brain and your muscles can become blocked, compromising your body’s ability to function as it needs to. Every chiropractor’s goal is to remove these subluxations, since they can both cause pain and impede feeling, Helfrich says.
But these fixes help more than just back pain. The lumbar region (your lower back) is a huge hub for the nerves that extend into your reproductive regions. Removing lumbar subluxations can improve nerve flow to your sexual organs, increasing things like blood flow to your clitoris or, for your husband, the penis.
The flow of nerve signals is a two-way street, though, meaning that adjustments also allow your organs to send messages to the brain more easily. This means that you not only do you become physically aroused faster, but your brain also registers that ready-for-action, heightened sense of pleasure more quickly, so you move past the mental obstacles that may be keeping you from orgasming, Helfrich explains.
The other key adjustment area for a better sex life? Right below your brain stem, around the vertebrae known as C1 and C2. “Libido and fertility require a delicate balance of estrogen, progesterone, and other hormones, many of which are released in the upper cervical and neck area,” he explains. If there are any blockages right out of the brain, the impingement up there will have an effect all the way down.
Even your fertility is affected by the nerves and hormones coming out of the spine, as they control your reproductive cycle.
But beyond all of the physiological benefits oftweaking your spine to perfection,
chiropractic adjustments can also simply give your muscles more range of motion. This means you can try previously impossible positions under the sheets.
“We want to improve people’s health, and health is about living life as its intended. Having a great sex life is huge part of that,” Helfrich adds. No arguments here!
CHIROPRACTORS HAVE CLAIMED FOR YEARS THAT WE CAN BE MORE COST-EFFECTIVE. BCBS HAS THE DATABASE THAT WOULD PROVE OUR THESIS, BUT THERE SEEMS TO BE A RELUCTANCE TO ALLOW OUR PROFESSION TO ACCESS THE DATA THAT WOULD PROVE US RIGHT.
In August 1999, Blue Cross/Blue Shield (BCBS) of Kansas presented a study titled “Lumbago Treatment.” This data was made available from a new program installed by BCBS called the McKesson Episode Profiler.
This program gave BCBS the ability to sort data according to specific diagnoses and compared the costs, frequency, and other factors between peer groups.
The data revealed that while less than eight percent of the study group were chiropractors, 38 percent of the patients chose to seek chiropractic care rather that allopathic medicine. This fact indicates that patients desire and are satisfied with the management techniques of the chiropractor.
The study did not include any hospitalization costs for surgery or any fees paid to orthopedists or neurosurgeons for costs associated with surgery. If the data included costs for these procedures, the savings for chiropractic would have been much greater.
When sorted by the average cost per episode, chiropractic is more cost-effective than anesthesiology; neurosurgery; neurology; registered physical therapy; orthopedic reconstructive surgery; physical medicine and rehabilitation; and rheumatology.
The greatest cost-effectiveness of chiropractic is demonstrated when one considers the global cost of allopathic care. The physical therapist can only receive referrals from an allopathic provider. An allopath can only write prescriptions. The allopathic provider primarily orders surgeries, nerve conduction tests MRIs, and CT scans. Hospitalization charges are totally allopathic charges that cannot be associated with chiropractic. When these charges are considered, the tremendous economy of chiropractic management becomes indelibly clear.
The majority of chiropractic charges were associated with the basic office-treatment-related services performed. Eighty-nine percent of the chiropractic charges were for services related to the treatment, while only 45 percent of the family practice costs were related to treatment of the condition. The remainder of the costs were for expensive diagnostics.
Patients who visit the family practice provider have about a 15 percent chance that they will have a MRI or CAT scan. These services cost an average of over $1,000 and provide no treatment, only a diagnosis.
For each 100 episodes, the chiropractor provided 265 modalities. For each 100 episodes, the registered physical therapist provided 885 modalities: over three times as many units of physical therapy provided by RPTs than chiropractors. This is a cost that has to be globally charged to the family practice providers, since patients cannot access RPTs without a referral from a medical doctor.
Registered physical therapists provided 303 office visits per 100 episodes, compared to 255 by the chiropractor. When RPTs are combined with the other allopathic portals, there are 598 office visits per 100 episodes. Therefore, the myth claiming chiropractors treat the patient more than the allopathic portals is obviously just diversionary, and not based on facts.
Patients had a willingness to return to the chiropractor that was 22 percent greater than the combined totals of allopathic portals. This indicates a level of satisfaction that is demonstrated by the patient’s willingness to return, based on results and confidence.
The BCBS lumbago study demonstrates that chiropractic is not only cost-effective but also quality effective. Adding chiropractic services would only decrease the cost to the plan. What is hard to explain is the prejudice against chiropractic in the design of BCBS plans, and their reluctance to push the study and analysis of the data to the next level. It almost seems as though there is a fear that exists in the minds of those in positions of power, preventing them from presenting the cost comparisons with the global cost of allopathic portals to chiropractic. Chiropractors have claimed for years that we can be more cost-effective. BCBS has the database that would prove our thesis, but there seems to be a reluctance to allow our profession to access the data that would prove us right.
I guess the million-dollar questions are “Why?” and “What are they afraid of?” Perhaps it is the fear of knowing how to handle the data once it proved that chiropractic was more cost-effective. Perhaps it is getting past the mindset that adding chiropractic benefits is going to increase reimbursement levels. Perhaps they cannot see that there would not be a cost increase but a cost savings from directing patients to more cost-effective portals. Allowing osteopaths to treat broken arms did not increase the number of fractures; it simply shifted the point of access to treatment. Likewise, allowing patients to freely access chiropractic services would not increase the number of spinal related injuries; it would simply allow the patient access to desired and more cost-effective services.
I imagine that BCBS of Kansas regrets releasing the amount of information they already have. There seems to be a reluctance to push the analysis of the data to the next level. It is now up to the profession to “hold their feet to the fire” and push for more data to support the fact that chiropractic can be more cost-effective.
Sciatica is best characterized as the common symptoms of pain and discomfort in the backs of the legs. This painful condition generally develops due to complications affecting the region of the lumbar spine, or lower back, affecting these areas of the body as well as an individual’s legs and feet. The pain which travels down the person’s legs through the sciatic nerves which are the nerves found surrounding the lumbar spine, characteristic of sciatica. The lumbar region of the spine is made up of five vertebrae which are labeled from top to bottom, L1 to L5, between the ribcage and the pelvis. Below these is the sacrum, which is labeled as S1. A spinal nerve can be found above each of these vertebra with its root in the spinal cord. These nerves form the sciatic nerve. The sciatic nerves, found in each leg, are the longest and broadest nerves found in the human body. When the root of one of the sciatic nerves becomes irritated or inflamed, leading to the compression of the nerve, it can cause the common symptoms of pain and numbness in the buttocks, legs, and/or feet.
A study conducted in an acute care facility in Hong Kong to determine the occurrence of back pain in nurses reported that 80.9% of the participating individuals suffered from some form of back pain throughout their careers with one third of them experiencing back pain at least once a month. The study also concluded that the contributing factors for back injuries among those nurses were caused from lifting and transferring patients, where stooping was recognized at the most common factor contributing to back complications. Most diagnosed cases of back pain were reported on orthopedic wards, closely followed by elderly or geriatric nursing. According to the study, back pain as a result of standing for extended periods of time was not considered significant. Another study conducted to determine the impact of back pain in nurses concluded that depression is associated with chronic low back pain and other symptoms which could exhibit as low morale and lower job performance among nurses. Additionally, the study also showed that two thirds of the nurse sample population suffered from back pain more than twice a year.
At Injury Medical & Chiropractic Clinic, chiropractor Dr. Alex Jimenez offers innovative options and improved assistance for people who have experienced an injury as a result of an auto accident. Dr. Jimenez can provide complete care for automobile accident victims by offering help with legal referral services as well as extended chiropractic options for treating common auto accident injuries, such as soft tissue injuries and whiplash. After being involved in an automobile accident, symptoms of back pain, neck pain, and headaches most commonly result soon after. Whiplash is a soft tissue injury frequently diagnosed after a car crash and results when a person’s body has absorbed the great force of two automobiles impacting into each other. The term whiplash is used to describe a wide variety of injuries of the neck caused by an abrupt and rapid, back and forth snapping motion of the head, such as when an individual is rear-ended in a car. The symptoms for whiplash can range from mild neck pain, stiffness, and discomfort to severe injury on the spinal cord, fractures, or dislocations.
Arthritis through degeneration, also known as osteoarthritis, results in the breakdown of the bone and cartilage of the spine over time from the natural wear and tear that comes with aging. Arthritis can occur in different areas of the spine causing impairing neck or low back problems but, among the different types of osteoarthritis, facet joint arthritis is among the most common of all the degenerative lumbar spine conditions. The joints are covered with articular cartilage that function jointly with the spinal disc spaces between each vertebra to allow movement and flexibility on the spine. Although, like other joints in the body covered with articular cartilage, the facet joint cartilage will breakdown as a result of degeneration which makes them more prone to be affected by arthritis.
Your low back pain could be caused by many reasons, characterized by the familiar symptoms of sciatica, but an additional pain, numbness, or tingling in both of your legs could be indicating another common condition associated with low back pain, lumbar spinal stenosis. Lumbar spinal stenosis is a progressive spinal condition identified by degenerative changes in the spine that lead to a narrowing of the spinal canal. Through time, the narrower spinal canal begins to pinch the spinal nerve roots causing the well-known low back pain.
|
Chiropractic spinal mobilization techniques involve the slow and steady movements of the spine's joints reestablishing their range of motion. Because it is a slower treatment style the techniques are done with the hands. However, a chiropractor can use various instruments/tools as well. Spinal mobilization treatment has the same focus as spinal manipulation. To get the body back to optimal health and allow the body to heal itself naturally. However, there can be a variety of reasons for utilizing spinal stabilization, with treatment depending on the patient's needs, if there are underlying conditions, or previous injury/s, and individual preference. Some prefer mobilization because it is gentler and does not generate the pops or cracking sounds. And the chiropractor's style/specialization comes into play. Some work in the firm manipulation high-velocity style, while others utilize the softer mobilization style and others work in combination. Manipulation High-Velocity Low-Amplitude Techniques This adjustment re-alignment utilizes the necessary force to release the joint out of its restricted motion to improve mobility and reduce pain. There are various types of high-velocity low-amplitude manipulation approaches. These are the more common manipulation techniques: Diversified Technique This high-velocity low-amplitude technique is the one that is commonly associated with chiropractic manual adjustments. The chiropractor applies a short - low-amplitude, quick high-velocity thrust of the restricted joints. This is done one at a time with the objective to restore the normal range of motion. The patient is positioned in various positions to optimize the adjustment/alignment. Gonstead Adjustment The Gonstead technique is another high-velocity low amplitude adjustment. It is similar to the diversified technique. The difference is the evaluation performed to specifically locate the painful joint and positioning of the body as the treatment is performed. Chiropractic or physical therapy chairs and tables can be used to position the patient for optimal treatment, like a cervical chair or a chest-knee table. Thompson Terminal Point Drop Technique Here specialized treatment tables with sections that drop down during a high-velocity low-amplitude thrust. The idea is that as the table drops the piece dropped allows for easier movement of the joint. A cracking sound can sometimes be heard. It depends on the patient and their condition. This type of manipulation can also be done in a gentle fashion making it a form of spinal mobilization. Spinal mobilization Slow steady motion/movements are performed to mobilize the joint. Spinal mobilization can be recommended for certain individuals for different reasons like: - Individual preference for spinal mobilization over spinal manipulation
- Individuals with a sensitive nervous system can benefit from the gentle technique. This can keep the body from experiencing a negative reaction that can cause muscle spasms or other issues.
- Individuals with certain conditions could be given a recommendation for spinal mobilization. This could be:
- Advanced osteoporosis
- Bone pathology
- Spinal deformity
- Types of inflammatory arthritis
- Individuals in the acute stage of their condition and experiencing severe pain
- Obesity can be a factor as the positioning and the manipulation procedures can be a challenge for the provider and the patient requiring a low force approach.
Mobilization Approaches The more common spinal mobilization approaches include: Activator Technique The Activator is a hand-held, spring-loaded tool that generates a low-force impulse. A patient lies face down on the adjustment table, while the chiropractor: - Examines leg length
- Performs muscle testing
- Adjusts the spine and/or extremity joints
Cox Flexion-Distraction Technique Here a gentle adjustment is designed to adjust the vertebrae by gently stretching the lower spine. This is usually performed in a series of repetitive slow movements like a steady rocking motion. Toggle Drop Here gravity is utilized to apply the adjustment. The chiropractors' hands are crossed and on top of each other. Then the chiropractor presses down quickly and firmly on the area of the spine while a section of the table drops. The table sections can be raised and dropped according to the localization of the spinal adjustment. McKenzie Technique This technique incorporates active patient involvement, empowerment, and self-care as part of the treatment. Spinal Release The chiropractor separates the misaligned vertebrae by applying gentle pressure using the fingertips, with the objective to restore the spine back to a natural position. Sacro-Occipital Technique - SOT This technique utilizes wedges/blocks under the pelvis. This allows gravity with added low-force to assist the chiropractor to realign the pelvis. Sciatica Alleviation All of these techniques can be utilized by a chiropractor for sciatic nerve pain alleviation or can discover other conditions that could be mimicking sciatica. Nerve mobilization techniques have been recently used as a method to adjust radiating pain related to disc disease, and in particular, mobilization techniques for the sciatic nerves improve mobility of the sciatic nerves, decrease mechanosensitivity of the nervous system, and heighten compliance of nerve tissues, relieving low back pain. Jeong, Ui-Cheol et al. “The effects of self-mobilization techniques for the sciatic nerves on physical functions and health of low back pain patients with lower limb radiating pain.” Journal of physical therapy science vol. 28,1 (2016): 46-50. doi:10.1589/jpts.28.46 Dr. Alex Jimenez’s Blog Post Disclaimer The scope of our information is limited to chiropractic, musculoskeletal, physical medicines, wellness, and sensitive health issues and/or functional medicine articles, topics, and discussions. We use functional health & wellness protocols to treat and support care for injuries or disorders of the musculoskeletal system. Our posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate and support directly or indirectly our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. We understand that we cover matters that require an additional explanation as to how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. The provider(s) Licensed in Texas& New Mexico*
Mindfulness is the most common treatment with the best supporting evidence towards improving and managing chronic pain. A recent study demonstrated that mindfulness-based stress reduction, or MBSR, including mindfulness meditation and other mindfulness interventions, can help reduce back pain and enhance psychological control by increasing brain blood flow to the frontal lobe. Practicing mindfulness involves activating a brain relaxation pathway by intentionally ignoring mental “chatter” and focusing on your breathing. Cognitive behavioral therapy, or CBT can also be helpful for chronic low back pain. Cognitive behavioral therapy can prevent an acute injury from progressing to chronic low back pain. Hypnosis may also help relieve chronic low back pain. However, CBT and hypnosis have weaker evidence to support their effectiveness on back pain.
A herniated disc, also known as a slipped or ruptured disc, is a healthcare condition which occurs when a tear in the outer, fibrous ring of an intervertebral disc causes its soft, central portion to bulge out from the damaged, surrounding cartilage. Disc herniations are generally due to the degeneration of the outer ring of an intervertebral disc, known as the anulus fibrosus. Trauma, lifting injuries or straining may also cause a herniated disc. A tear in the intervertebral disc may result in the release of chemicals which may cause irritation and ultimately become the direct cause of severe back pain, even without nerve root compression. Disc herniations also commonly develop following a previously existing disc protrusion, a healthcare condition in which the outermost layers of the anulus fibrosus remain intact, however, these can bulge if the disc is placed under pressure. Unlike a disc herniation, none of the gel-like section escapes the intervertebral disc. Herniated discs often heal on their own within several weeks. Severe disc herniations may require surgery, however, a variety of research studies have demonstrated that nonoperative treatment may help improve and manage the recovery process of a herniated disc without the need for surgical interventions.
Several lumbar spine (lower back) disorders can cause sciatica. Sciatica is often described as moderate to intense pain at the left or right leg. Sciatica is caused by compression of at least one of the 5 places of nerve roots in the lower spine. Sometimes physicians call a radiculopathy sciatica. Radiculopathy is a term used to refer to pain, numbness, tingling, and weakness in the arms or legs brought on by a nerve root issue. If the nerve problem is in the neck, then it is called a cervical radiculopathy. However, because the low back is affected by sciatica, it is called a lumbar radiculopathy. Five sets of nerve roots at the lumbar spine combine to produce the sciatic nerve. Beginning at the back of the pelvis (sacrum), the sciatic nerve runs from the trunk, beneath the buttocks, and downward through the hip place into every leg. Nerve roots aren’t “solitary” structures but are a part of the body’s entire nervous system capable of transmitting pain and sensation to other areas of the human body. Radiculopathy occurs when compression of a nerve due to a disc rupture (herniated disc) or bone spur (osteophyte) occurs in the lumbar spine prior to it joining the sciatic nerve.
Chiropractors use a string of treatments designed to manipulate tissues of the entire body, joints, and the spine to alleviate pain and improve functional ability. Usually, this will be referred to as spinal manipulative therapy (SMT), but you’ll find many other chiropractic treatment procedures.
A chiropractor tailors her or his treatment approach based on the individual needs of a patient, utilizing a traditional doctrine of starting off together with the more natural, less-invasive therapies before continuing to some more aggressive approaches.
At each stage throughout the process, chiropractors preserve a strict emphasis on communicating together with the patient precisely what’s going to happen. The chiropractor makes sure the patient comprehends everything that happens during a diagnosis, evaluation, and also the planned procedures, to be able to educate the patient and receive direct acceptance to commence the treatment process. This emphasis on informed consent is vital because stuff threat*, which means there could a danger, however, unimportant, that a certain process perhaps could cause an injury may be carried by some chiropractic techniques.
Around 80% of the population is plagued at one time or another by back pain, especially lower back pain. Associated leg pain (called lumbar radiculopathy or sciatica) happens less frequently. Pain could be debilitating and bothersome, restricting daily activities. Leg and back pain can result from a number of reasons, not all of which originate in your spinal column.
With the aim of this particular article, we’ll concentrate on lumbar radiculopathy, which refers to pain in the low extremities in a dermatomal pattern (see picture below). A dermatome is a special place in the lower extremity that’s nerves going from a particular lumbar nerve to it. Compaction of the origins of the spinal nerves in the lumbar region of the back causes this pain. Diagnosing leg and lower back pain begins with assessment and a detailed patient history.
“Doctor, are chiropractic adjustments safe?”
This is one of the most common questions asked by people seeking or considering chiropractic care along with
“What are the risks?”
“Can I receive spinal adjustments without the chiropractor adjusting my neck?”
“Do chiropractic adjustments cause arthritis or even strokes?”
With media scrutiny over natural health procedures, specifically chiropractic and cervical adjustments, these are very important and serious questions, especially when one’s health is a priority. As a practicing chiropractor, I welcome the opportunity to address these questions. Chiropractic care is profoundly safe, and this article summarizes the current research, providing answers to these common questions and misconceptions.
Myths vs. Facts
In 1990, when I started working in the chiropractic profession, a common concern that patients had about chiropractic care was that “too many adjustments would cause arthritis.” Years later, science has affirmed what chiropractors have always seen and known to be true in clinical practice – that in fact chiropractic care is not only one of the most popular forms of care for people with arthritic conditions but one of the most effective.1,2
Unfortunately, for hundreds of years, health care practices have been permeated by folklore, sometimes known as “old wives tales.” The trend continues today. A 2010 study of over 1,000 board-certified American pediatricians found that over 75% of the doctors subscribe to at least one known health care myths.3 These include the myths that eating chocolate causes acne, listening to Mozart will make a baby smarter, and swimming within 30 minutes of eating is not safe. Many doctors in this study were also found guilty of not knowing the expected protocols for treating burns, healing wounds, administering Aspirin to children, and safely dealing with seizures.
A review of the current literature indicates that frequent or extreme complications of chiropractic care should also be included in the list of the most common medical myths prevalent even in our medical offices.
Spinal Care vs. Chiropractic Care
The spinal column’s role in overall health cannot be undermined as it houses the brainstem, spinal cord, and central nerve system. Thus, for optimal health the spinal column must be examined and cared for by a skilled doctor.
Specifically, the foundation of chiropractic care teaches that damage to the spine, and misalignments of the vertebrae (subluxations) create interference in the nerve system, which are therefore reduced and corrected through specific chiropractic adjustments.4,5
On that basis, chiropractic adjustment techniques have historically been rooted in precision and accuracy. Although there are now many unique chiropractic techniques taught in professional schools and in continuing education, these techniques commonly focus on the evaluation and measurement of subluxation patterns in the spine and the specific protocols used to reduce the areas of misalignment. In contrast, most other health care practices addressing the spine, never mind non-medical procedures attempted at home, are for the most part, generalized treatments of pain, global mobilizations of joints, and overall tractions of entire regions of the spinal column.
Receiving a specific chiropractic adjustment to reduce a subluxation is immensely different from receiving any form of “treatment” on the spine. Admittedly, I did not understand this practice in my first 20 years of receiving chiropractic adjustments. Until I attended chiropractic school and learned the techniques and analyses used in chiropractic science, I thought that chiropractic adjustments were all one-of-the-same. I can understand how the general public might also construe this misconception – I did and I grew up in a chiropractic family. Subluxations and adjustments are specific; the more extensive the analysis used by the chiropractor, the more precise the adjustment, and thus the better improvement in the patient’s health.
In my experience, the majority of the “chiropractic horror stories” shared in folklore, and even many of the cases cited by medical research, fall into one of two categories:
(a) The case of a the patient receiving care without extensive and correct analysis
(b) A person receiving spinal care incorrectly identified as “chiropractic care” administered by someone other than a licensed Doctor of Chiropractic
In fact, a 1995 report in the Journal of Manipulative and Physiological Therapeutics revealed that many “manipulations,” incorrectly attributed to chiropractors, had been rendered by non-chiropractic professionals including GPs, osteopaths, and physiotherapists, and even laypeople including a wife, a Kung-Fu practitioner, a blind masseur, and an Indian barber.6,7 Therefore before someone suggests they were hurt or injured by a “chiropractor,” it is imperative to learn more about their experience. In all likelihood some level of scrutiny was overlooked – or they weren’t seeing a licensed chiropractor at all.
Modern chiropractors use advanced technological analyses such as X-ray, surface electromyography (sEMG), thermography, and digital postural analysis, along with traditional chiropractic methods of motion and static palpation, leg length analysis, and visual postural inspection to make a diagnosis and determine the appropriate adjustment. Naturally, to use layman’s terminology, if a patient presented to the chiropractor with a low left hip, and the chiropractor adjusted the left hip “even lower,” the patient would get worse. For this reason, your Doctor of Chiropractic is not only highly trained but expected under every state and provincial law to thoroughly assess your spine and condition prior to making recommendations or giving adjustments.
What about stroke?
Since the 1990s, the most extreme fallacy about chiropractic care is that “adjustments of the cervical spine cause strokes.” As a practitioner, I am pleased to observe greater inter-professional cooperation between physicians and chiropractors, but I am disappointed by the increasing number of patients who have consulted me following a discussion with their medical doctor and told to “not get their necks adjusted.”
A basic understanding of the origins of chiropractic care, and the critical function, anatomy, and physiology of the central nerve system demonstrates why the suggestion that patients should “not get their necks adjusted” is absurd. While chiropractors are concerned with the reduction of nerve system stress caused by spinal subluxations throughout the entire spine, one must understand that all spinal nerves first pass through the upper cervical spine. Therefore, interference to the nerves passing from the brain through the spinal cord to any area of the body could occur either at the associated spinal segment where the peripheral nerve exits the spinal column, or at any place higher, including the upper cervical spine. Historically, Dr. B.J. Palmer, who developed the modern chiropractic profession, focused the majority of his research and efforts into the reduction of upper cervical spine subluxations, expressing that upper cervical subluxations were the foremost cause of disease and dysfunction compared to other subluxations in the spine.8 Years later, science continues to affirm the importance of upper cervical alignment. It has been demonstrated that abnormal cervical alignment is a leading cause and an almost universal finding related to not only cervicogenic pain and headaches, but also the development of scoliosis9,10 and even sudden infant death syndrome (SIDS).11.12,13 This awareness of the basic physiology of the nerve system is enough to understand the utmost importance of reducing subluxations in the cervical spine, above all other areas of the nerve system.
The “stroke hypothesis” stems from the theory that the irritation of the vertebral arteries, which pass through the cervical vertebrae, could lead to an ischemic stroke by causing accumulated plaque in the arteries to be dislodged. As strokes may cause serious, permanent impairments in a person’s health, there has naturally been much interest and research in this topic.
Consider how plaque develops in the arterial system of the body. Exposure to the known risks of poor diet, alcohol consumption, and smoking over a period of many years may cause molecular plaquing in the arteries, and it is true that when those molecules become dislodged, they can affect the brain, which is known as a stroke. Unfortunately, your family doctor or your chiropractor can’t prevent this from happening – you would need immediate emergency medical attention in hospital to prevent this from occurring.
Warning signs that a stroke may be about to occur include upper back pain, neck pain, and headaches. Naturally, people dealing with these symptoms may consult their chiropractor, hoping for a resolution of pain. Many may also consult their MDs and/or other trusted health care providers. Unfortunately, such pre-stroke symptoms as back pain, neck pain, and headaches may not explicitly appear to be the early stages of a vascular incident without the “red-flag” accompanying symptoms of blurred vision, dizziness, slurred speech, facial drooping, and lack of coordination. Therefore, as it is not standard practice for chiropractors or medical physicians to refer every case of back pain or headaches to the emergency room, patients may receive chiropractic or medical intervention without knowing that a stroke is ensuing.
When is a chiropractor or medical doctor negligent? If a patient visits the doctor’s office with neck pain and headaches while showing the classic signs of stroke (slurred speech, dizziness, poor coordination, etc.), the doctor is obligated to identify this and ensure that a stroke is not about to happen. If, after examination, a doctor identifies that a stroke may be forthcoming, the doctor must see that the patient receives the necessary immediate medical attention. Doctors who do not rule out the possibility of an imminent stroke or do not ensure necessary medical attention if a stroke is indeed forthcoming, would indeed be negligent – but this is very far from “causing” the person’s stroke, whether or not any treatment was rendered.
In fact, although a chiropractic adjustment would not slow down the incidence of the stroke, 2008 research shows that it would no more accelerate it than a visit to the medical doctor. In an article published in SPINE, a multi-disciplinary team of researchers found that while strokes are very rare events in the general public, there was only an increased correlation between chiropractic visits and the occurrence of stroke, due to patients with headaches and neck pain seeking care before their stroke.14 Notably, the correlation of medical visits and strokes matched that of chiropractic visits and strokes; neither form of care was shown to increase the risk of stroke. In either case, the unfortunate patient was headed for a vascular incident. The occurrence of a stroke after a visit to the chiropractor (or the medical doctor) provides no association of cause, only correlation.15
Is your chiropractor required to warn you about the possibility of a stroke with a chiropractic adjustment? Interestingly, Dr. Christopher Kent, who is an attorney, independent researcher, and president of the Foundation for Vertebral Subluxation, has expressed that “such informed consent must be based on appropriate information and since there is no scientific evidence that chiropractic adjustments or neck manipulations actually cause strokes, it is inappropriate to require a doctor to suggest that such a risk exists.”16 Nevertheless, most state and provincial laws require Doctors of Chiropractic to disclose a remote risk of stroke to their patients, for this is common practice for “material risks” even when the likelihood of occurrence is very small.17
Long-term Benefits of Chiropractic Care
Rather than study isolated reports of adverse incidences which may (or may not) occur within one visit to the chiropractor, it is more revealing to measure the long-term benefits of chiropractic care. Ultimately, studies consistently demonstrate that a healthier spine relates to a healthier person.
Beyond symptomatic relief, a growing number of chiropractors place emphasis on corrective care and spinal hygiene, to maintain and promote the health of the spinal column and nerve system.
Without maintenance of spinal health, we now know through numerous studies that posture misalignment not only affects neurology but also the vascular system. A 2004 study revealed that older men and women with hyperkyphotic postures have increased rates of death, specifically associated with increased atherosclerosis.18 With atherosclerosis increasing the incidence of an ischemic stroke, it is only logical for health-conscious individuals trying to prevent strokes to maintain healthy posture through chiropractic care.
Further, whereas a 2005 study showed that the reversal of the normal cervical curvature results in vascular changes in the spinal cord,19 the maintenance of this proper alignment should be of highest importance to those interested in the prevention of vascular incidents.
Statistically, the incidence rates favour those individuals receiving chiropractic care. In 1995, the Journal of Manual and Physiological Therapeutics published the risk of fatal stroke associated with chiropractic cervical adjustments. Although no cause was shown in the article, the correlation is estimated to be 1 in 400,000 or 0.00025%.20 Newer studies suggest the risk may be as low as 1 in 6 million, 0.00002%.21 Notably, the National Center for Health Statistics indicates the mortality rate from stroke in the general population is more than twice the rate of the most conservative estimates correlating chiropractic. The risk in the general population is 1 in 175,000 or 0.00057%.22
Not only is the risk of death from stroke after a cervical adjustment substantially less than the risk of fatal stroke in the general population, other long-term studies of chiropractic patients have shown:
Improved lung capacity, athletic ability, and vision23
Better functional capacity, and reduced relapse of prior disability24
Better overall health and greater activity levels25
Enhanced DNA repair and enzyme activity; reduced impact of oxidative stress26
Fewer hospital visits, reduced pharmaceutical costs, and medical expenditures27
Improvement in health, wellness, and quality of life28,29
The Final Verdict: Malpractice Claims
Lastly, as it is always possible that research could be slanted based on who was conducting it, perhaps the best measures of safety are the malpractice insurance costs for chiropractors and the actual frequency and success of claims filed against them. No one pays closer attention to injury statistics than Malpractice Insurance carriers.
According to the Canadian Medical Protective Association, annual malpractice rates for Ontario medical doctors range from $1,572 for the family physician and $7,332 for the neurologist, to $44,520 for the Obstetrician.30 By comparison, the Canadian Chiropractic Protective Association’s standard rate for chiropractic malpractice insurance is less than $1,300 per year. Notably, the first-year doctor of chiropractic is extended a new member discount of approximately 50% (as opposed to an increased premium), not reflecting any greater risk for a patient seeing a doctor with less experience.31
American rates reflect the inter-professional differences to an even greater degree. Whereas the U.S. physician could pay $25,000 to $50,000 per year for malpractice coverage, U.S. chiropractors pay annual rates less than $5,000.32,33 The chiropractic profession has a well-established record of safety and efficacy, and the chiropractor’s malpractice insurance rates remain among the lowest across health professions.34 The varying rates are directly related to the risk involved in the doctors’ procedures, the claims filed against them, and the likelihood of future lawsuits.35
Although they are sensationalized in the media when they do occur, claims against chiropractors are very rare. Your chiropractor’s office consistently proves itself to be one of the safest health care facilities you can choose for your family.
Moving Forward
Unquestionably, there have been decades of misinterpretations, and unfortunately chiropractic myths have been passed down through generations. Certainly, professional bias has also played a role in the public’s misunderstanding of the safety and efficacy of chiropractic care. (The U.S. Court of Appeals determined in 1990 that the American Medical Association had engaged in a “lengthy, systematic, successful and unlawful boycott” designed to restrict cooperation between medical doctors and doctors of chiropractic.36) Fortunately, we are long past that day. What you would hope to find in the 21st century are cooperative teams of health care professionals working together for your benefit.
My personal recommendation is to seek a chiropractor who not only uses current technology and techniques to analyze and render care to his or her patients, but also is willing to engage in dialogue with your other health care providers. I recommend the same when choosing an M.D.
With this better understanding of chiropractic myths and the benefits of maintaining a healthy spine, I trust that you can comfortably move forward, integrating chiropractic care into your wellness lifestyle.
New Study Reports Substantial Growth in the Use of Chiropractic Care by the Department of Veterans Affairs
The Foundation for Chiropractic Progress (F4CP) notes that for more than 10 years, the U.S. Department of Veterans Affairs (VA) has included chiropractic services as part of the standard medical benefits package offered to all enrolled veterans. According to a new study conducted by researchers from the VA Connecticut Healthcare System, published in the Journal of Manipulative and Physiological Therapeutics, the use of chiropractic services and the chiropractic workforce in VA has grown substantially since their introduction over a decade ago. The annual number of chiropractic visits has increased by nearly 700 percent, thus demonstrating more veterans have access to chiropractic care than ever before.
“Our work shows that VA has steadily and substantially increased its use of chiropractic services each year following their implementation in late 2004,” states lead author of the study Anthony J. Lisi, DC, Director of the VA Chiropractic Program, and Chiropractic Section Chief at the VA Connecticut Healthcare System. He adds, “VA chiropractic care includes evidence-based, patient-centered treatment options that are in demand by veterans and referring providers. VA continues its efforts to ensure appropriate access to chiropractic care across the whole system, but as this paper shows, the progress to date has been remarkable.”
Among the multitude of findings during an 11 year period, the study showed that:
■ The annual number of patients seen in VA chiropractic clinics increased by 821 percent.
■ The annual number of chiropractic visits grew by 693 percent.
■ The total number of VA chiropractic clinics climbed 9 percent annually, and the number of chiropractor employees increased by 21 percent annually.
■ The average VA chiropractic patient is male, between the ages of 45 and 64, is seen for low back and/or neck conditions, and receives examination, chiropractic spinal manipulation and other health care services.
Co-Author Cynthia A. Brandt, MD, MPH, Health Services Researcher at the VA Connecticut Healthcare System and Professor at Yale University School of Medicine states, “Chiropractic care is an important component in the treatment of veterans with spinal pain conditions. The trends we identified provide a foundation for further research to examine the optimal models of care delivery for patients.”
The study notes: “Our results indicate that VA chiropractic clinics saw a greater percentage of female and younger patients compared with the national VA outpatient population. This demographic tendency is consistent with the cohort of veterans from the recent conflicts in Iraq and Afghanistan, which is known to have a high prevalence of musculoskeletal conditions.”
An Army report recommended the use of alternatives to pain drugs, including chiropractic care, massage and acupuncture. Here, Dr. Frank Lawler gives Spc. David Ash chiropractic treatment, January 7, 2011, in Tacoma, Washington. (Mark Harrison/Seattle Times/MCT)
“The growing utilization of chiropractic services among veterans for pain management and other health concerns, particularly those in the Operation Enduring Freedom, Operation Iraqi Freedom, Operation New Dawn and older adult populations, showcases the clear-cut demand for chiropractic care and is a direct reflection of the improved clinical outcomes and high patient satisfaction scores that have been documented previously,” says Sherry McAllister, DC, executive vice president, F4CP. “We commend VA for its participation in ongoing chiropractic research to help further improve the health and well-being of our respected and valued veterans.”
The authors also state that the growth in VA chiropractic use has occurred without additional laws mandating expansion. This suggests an increasing recognition of the value of chiropractic care in VA. In a recent editorial, VA Under Secretary for Health, David J. Shulkin, MD, cited VA’s chiropractic program as one example of the important health care expertise provided to veterans.
Doctors of chiropractic (DCs) – who receive a minimum of seven years of higher level education – provide non-operative management of conditions such as headaches, back pain, neck pain, or pain in joints, via a comprehensive approach including manual techniques and active rehabilitation. Chiropractic services are integrated with primary care, specialty clinics and rehabilitation, and provide a non-pharmacologic option for pain management, as well as general health and wellness concerns.
About Foundation for Chiropractic Progress:
A not-for-profit organization, the Foundation for Chiropractic Progress (F4CP) informs and educates the general public about the value of chiropractic care. Visit www.f4cp.com or call 866-901-F4CP (3427). Social media: Facebook, Twitter, LinkedIn, Pinterest, YouTube.
View source version on businesswire.com: http://www.businesswire.com/news/home/20160620005430/en/
Nurses nowadays encounter the common question on how they can prevent or even manage lower back pain. In fact, back complications are one of the most reported occupational health complications for nurses, especially through their retirement years. Many healthcare workers resort to self-medicating with over-the-counter pain relievers but, while these may offer relief from their symptoms, the effects are only temporary. Through several lifestyle changes, many nurses could achieve long-term relief from their lower back pain by managing their symptoms and prevent further low back complications. First, stretching and exercising regularly should be fundamental for a nurse. Staying in a single position for long periods of time, as it’s usual in the healthcare workplace, can place an unequal amount of pressure on the muscles, resulting in muscle weakness and uneven distribution of weight. Stretching frequently on the job can help loosen up tight muscles and temporarily relieve back pain. Then, following a series of stretches with exercise can help regulate and further reduce back pain because it strengthens the structures supporting the back muscles. Engaging in strength training exercises can help keep low back pain away longer. Additionally, stretching and exercising the body enough before symptoms of back pain appear in the fist place can also help prevent back complications from developing.
The piriformis muscle, a small muscle located deep in the buttocks, plays the important role of rotating the legs outwards. Piriformis syndrome is a painful condition that occurs when the piriformis muscle becomes too tight, compressing the sciatic nerve that runs through the buttocks. Characterized by symptoms of pain, tenderness, and occasionally, numbness around the area of the buttocks, piriformis syndrome symptoms may also expand down an individual’s leg including the calf. Piriformis syndrome can be caused by several reasons but there are two frequently notable causes for the condition. First, sitting for extended periods of time can cause the piriformis muscle to tighten. Second, an accident resulting in direct injury such as a fall or a sports-related injury can damage the piriformis muscle. Trauma to this muscle in the buttocks can cause the surrounding tissue to become inflamed and swollen, leading to compression and possible irritation of the sciatic nerve. Muscle spasms can also cause piriformis syndrome. Usually starting as a muscle strain, a muscle spasm can occur abruptly and cause pain. However, the source of muscle spasms can frequently be unknown. Regardless of the initial cause, being aware of your treatment options for piriformis syndrome is essential towards alleviating the painful symptoms and healing the condition.
While low back pain is remarkably common, the issues are caused by a variety of conditions or injuries involving the intricate network of spinal muscles, nerves, bones, discs, or tendons in the lumbar spine. An affliction to any of the local structures of the lumbar spine can result in radiating pain that may travel to other parts of the body but the symptoms and severity of low back pain vary greatly for each individual. These are 5 common conditions that could be the source of your low back pain.
The irritating pain that accompanies tight muscles along with limited mobility and the numbness that extends down your buttocks and legs are the all too familiar symptoms associated with low back pain relating to conditions of the lumbar spine. But, when your lumbar back pain points to the sacroiliac joint instead, what are your treatment options? The function of the sacroiliac joint is to support the movements of the lower extremities. With overuse or underuse, the local muscles surrounding the joint may become inflamed or tight, adding pressure and stress that will often lead to sacroiliac joint dysfunction, the possible true cause for your low back pain.
|



 Your new post is loading...
Your new post is loading...






















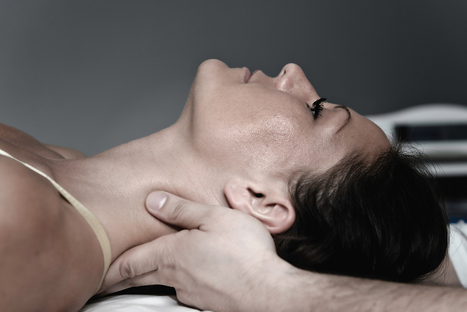









Poor posture becomes a habit that goes on until discomfort or pain present. Body awareness is known as proprioception. Chiropractic can help. For answers to any questions you may have please call Dr. Jimenez at 915-850-0900 or 915-412-6677